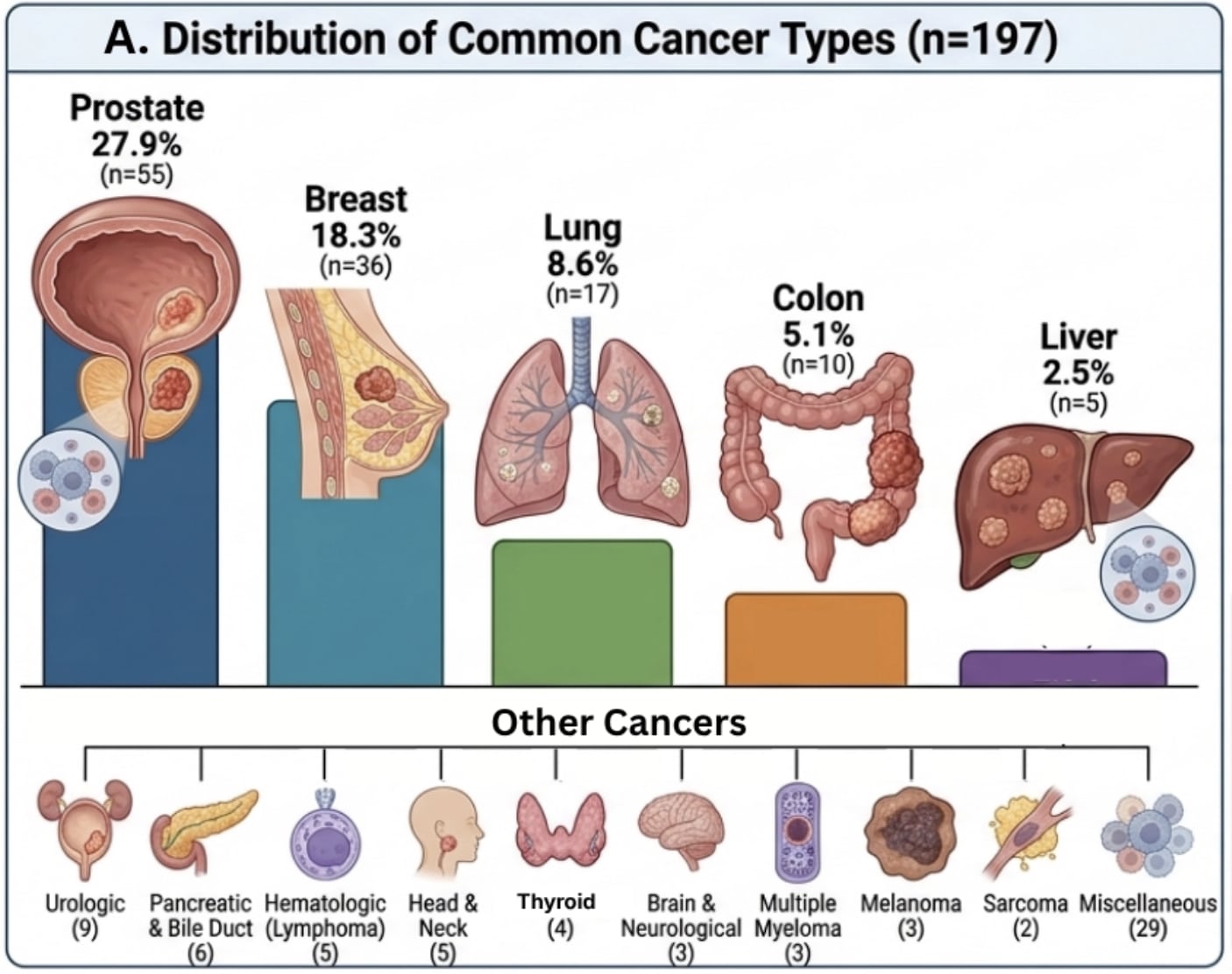
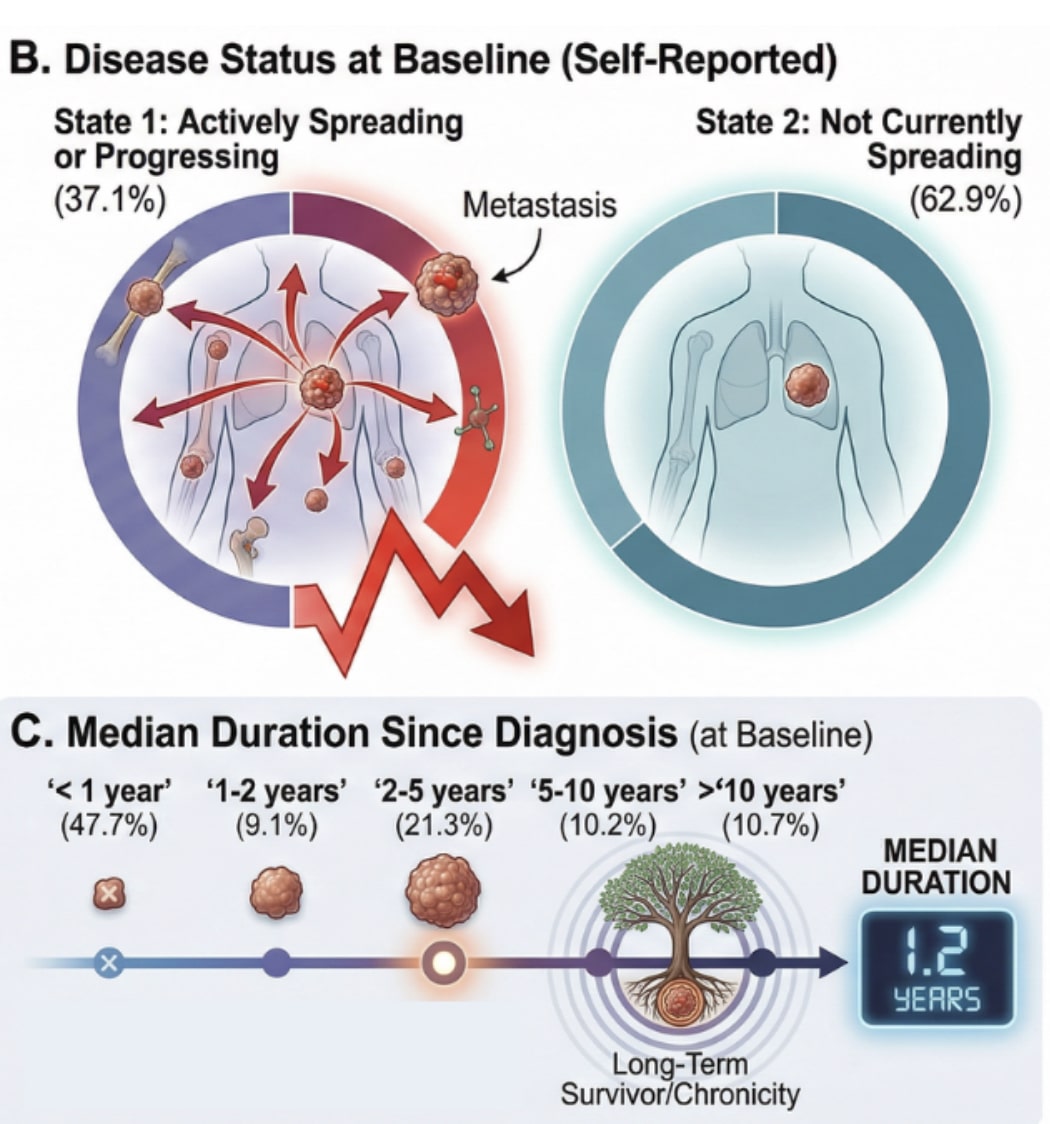
Menopausal Hormone Therapy for the Primary Prevention of Chronic Conditions: A Systematic Review to Update the U.S. Preventive Services Task Force
Background: Menopausal hormone therapy to prevent chronic conditions is currently not recommended because of its adverse effects.
Purpose: To update evidence about the effectiveness of hormone therapy in reducing risk for chronic conditions and adverse effects, and to examine whether outcomes vary among women in different subgroups.
Data Sources: MEDLINE (January 2002 to November 2011), Cochrane Central Register of Controlled Trials and Cochrane Database of Systematic Reviews (through the 3rd quarter of 2011), Scopus, and reference lists.
Study Selection: Randomized, placebo-controlled trials of menopausal hormone therapy published in English since 2002 that assessed primary prevention of chronic conditions.
Data Extraction: Investigators extracted data on participants, study design, analysis, follow-up, and results; 2 investigators independently rated study quality by using established criteria.
Data Synthesis: 9 fair-quality trials met the inclusion criteria. The Women’s Health Initiative reported most of the results, had 11 years of follow-up, and had data most applicable to postmenopausal women in the United States. It showed that estrogen plus progestin reduced fractures (46 fewer per 10 000 woman-years) and increased invasive breast cancer (8 more per 10 000 woman-years), stroke (9 more per 10 000 woman-years), deep venous thrombosis (12 more per 10 000 woman-years), pulmonary embolism (9 more per 10 000 woman-years), lung cancer death (5 more per 10 000 woman-years), gallbladder disease (20 more per 10 000 woman-years), dementia (22 more per 10 000 woman-years), and urinary incontinence (872 more per 10 000 woman-years). Estrogen-only therapy reduced fractures (56 fewer per 10 000 woman-years) and invasive breast cancer incidence (8 fewer per 10 000 woman-years) and death (2 fewer per 10 000 woman-years) and increased stroke (11 more per 10 000 woman-years), deep venous thrombosis (7 more per 10 000 woman-years), gallbladder disease (33 more per 10 000 woman-years), and urinary incontinence (1271 more per 10 000 woman-years). Outcomes did not consistently differ by age or comorbid conditions.
Limitation: Limitations of the trials included low adherence, high attrition, inadequate power to detect risks for some outcomes, and evaluation of few regimens.
Conclusion: Estrogen plus progestin and estrogen alone decreased risk for fractures but increased risk for stroke, thromboembolic events, gallbladder disease, and urinary incontinence. Estrogen plus progestin increased risk for breast cancer and probable dementia, whereas estrogen alone decreased risk for breast cancer.
Primary Funding Source: Agency for Healthcare Research and Quality.
+Author Affiliations: From Oregon Evidence-based Practice Center, Oregon Health & Science University, and Providence Cancer Center, Providence Health & Services, Portland, Oregon.
1. Heidi D. Nelson, MD, MPH;
2. Miranda Walker, MA;
3. Bernadette Zakher, MBBS; and
4. Jennifer Mitchell, BA